Sensors make sense, facilitating frequent monitoring and keeping people with diabetes safe in hospital.
The Diabetes Technology Network (DTN-UK) has announced that, following a request to Abbott Diabetes Care from the DTN, Abbott’s Diabetes Care division have donated 6,500 FreeStyle Libre sensors to be used by NHS Trusts during the Covid-19 pandemic. The announcement was made by Dr Pratik Choudhary, Chair DTN – UK, and Dr Dinesh Nagi, Chair Association of British Clinical Diabetologists (ABCD).
There are two main purposes for this donation. First, to facilitate safe and rapid discharge of insulin- treated patients from hospital, allowing remote monitoring of glucose values post discharge in a scenario where there has been need for rapid changes in insulin doses, such as new diagnosis of Type 1 diabetes. Second, to protect patients as well as health care professionals by providing a means of contactless glucose monitoring during hospital stays where frequent glucose monitoring is required.
The use of two sensors (each lasts 14 days) per patient will allow these patients to be followed up remotely, keeping them safe and allowing the team to adjust insulin doses if required. At the end of the four-week period (two sensors) those patients who may meet current local guidelines for Libre may continue to use sensors. Other patients will need to be transferred to alternate modes of glucose monitoring according to local guidelines. The patient must have a compatible IOS or Android mobile phone to work with FreeStyle LibreLink, allowing for immediate HCP remote monitoring. The Trust will need to be set up with a LibreView account if one is not in place already.
Dr Choudhary said of the donation, “Recent data show that people with diabetes have an elevated risk of adverse outcomes with Covid-19, which is also linked to their glucose control. We are really pleased that Abbott has agreed to our request to help us support patients with diabetes who are admitted to hospital by donating FreeStyle Libre sensors. The use of the FreeStyle Libre system will facilitate frequent monitoring of glucose for those who need it to control their blood glucose. It also allows us to view patient data remotely, supporting timely discharge with safe and effective remote follow-up.”
Neil Harris, general manager of Abbott’s diabetes care business in the UK and Ireland adds, “Providing frontline healthcare professionals and patients with technology and equipment is critical in the fight against Covid-19. We’re delighted to make FreeStyle Libre sensors available for hospitalised people living with diabetes, which will help frontline healthcare workers to monitor and manage the glucose levels of these patients better and, at the same time, help limit Covid-19 exposure, helping to keep people safe.”
DISCHARGE
 Sometimes being discharged from hospital can feel confusing or feel a little anxious. A new leaflet produced by Diabetes UK and ABCD lets you know what to expect when you are discharged. There are also handy tips on things to think about after leaving hospital to ensure you stay as safe as possible. There are specific information on what you should expect on discharge and what the hospital should supply you with. Then there are things you’ll need to think about after leaving hospital including: medication, hypos, blood glucose monitoring, how to handle illness, ketones and a reminder to look after your feet.
Sometimes being discharged from hospital can feel confusing or feel a little anxious. A new leaflet produced by Diabetes UK and ABCD lets you know what to expect when you are discharged. There are also handy tips on things to think about after leaving hospital to ensure you stay as safe as possible. There are specific information on what you should expect on discharge and what the hospital should supply you with. Then there are things you’ll need to think about after leaving hospital including: medication, hypos, blood glucose monitoring, how to handle illness, ketones and a reminder to look after your feet.
There’s some info on what you might need to consider if you are new to insulin therapy, as well as who to contact to get follow-up support. The content was written by a national team of clinical experts and designed by the Leicester Diabetes Centre.
NEW SUPPORT
The NHS has launched new online support for people with diabetes with tools now available on the NHS in order to help people manage their condition during the coronavirus pandemic. Three new services allow people to manage their condition online, with a range of online videos and training available on apps designed for both children and adults.
Recent findings show that people with diabetes face a significantly higher risk of dying with Covid-19 but better management of the condition can help improve control and lead to better outcomes. NHS investment in the technology means that patients will be offered advice on treatment and care, as well as training to adopt healthy behaviours on diet and exercise. This remote support will complement patients’ appointments, many of which have been going ahead throughout the pandemic, through video consultations or via telephone, and more recently in Covid protected areas. There are already online appointments, routine discussions with GPs and a dedicated helpline for those treated with insulin so that diabetes care can go ahead as normal.
Digibete: Children and young people with Type 1 diabetes and their families will be able to use the DigiBete App and website for a wide range of awareness, education, training and support resources.
MyType1Diabetes: Adults with Type 1 diabetes can access the service directly by visiting myType1diabetes.nhs.uk, it includes videos and eLearning courses, to help people understand more about their Type 1 diabetes and increase their confidence in how to manage it.
The NHS Diabetes Prevention Programme is also being delivered remotely using platforms such as Microsoft Teams to continue to help those at risk of Type 2 diabetes to reduce their risk.
Professor Partha Kar, national specialty advisor on diabetes for NHS England and Improvement commented, “NHS has taken action to help people and keep them safe, including the roll out of these helpful apps. Access to trusted information and support is key to helping people manage their diabetes and we are delighted to support these tools which will hopefully empower people to look after their own condition and reduce their risk.”
LIFE SPORT DIABETES
Mel Stephenson-Gray’’s home workout circuit consists of 6 different exercises. She explains, “With each exercise we’ll do consecutively for 30 seconds and then rest for 30 seconds. If someone is new to fitness or this type of activity, they might choose to take a longer rest between each exercise, for say a minute or two. Once all of the exercises are completed, we then take a six-minute rest (which again is adaptable) and once recovered, we repeat the circuit all over again.”
She says, “This type of fitness session is inspired by the type of session I’ve often done with my training group over the years, particularly at the start of the winter or summer training season, as it helps build strength and fitness as a foundation to move onto other things. It works the arms, legs and core areas throughout the session, which can be helpful when training a lot, because no one area is necessarily over-worked or strained.”
The home workout videos have been accepted by many in the community. She adds, “I’m sharing what training sessions work for me. Please remember that you know your own fitness, health and diabetes best. Seek medical advice if you are concerned about undertaking physical activity.”
Micropatch potential
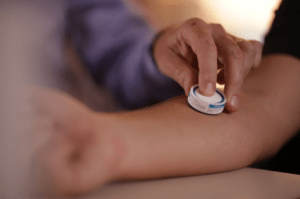 Merck has exercised its option to use Vaxxas‘ High Density Microarray Patch (HD-MAP) platform as a delivery platform for a vaccine candidate. The companies did not disclose what the vaccine candidate is supposed to treat. But Merck this month announced two Covid-19 vaccine development efforts: a collaboration with IAVI and plans to acquire vaccine developer Themis Bioscience. Vaxxas notes that any vaccine could be delivered with its dime-sized patch. Based on technology originally developed at the University of Queensland, Vaxxas’ HD-MAP includes a 9-by-9 mm array of thousands of very short projections around 250 microns in length. Invisible to the naked eye and coated with vaccine, the projections can quickly deliver vaccine to immune cells.
Merck has exercised its option to use Vaxxas‘ High Density Microarray Patch (HD-MAP) platform as a delivery platform for a vaccine candidate. The companies did not disclose what the vaccine candidate is supposed to treat. But Merck this month announced two Covid-19 vaccine development efforts: a collaboration with IAVI and plans to acquire vaccine developer Themis Bioscience. Vaxxas notes that any vaccine could be delivered with its dime-sized patch. Based on technology originally developed at the University of Queensland, Vaxxas’ HD-MAP includes a 9-by-9 mm array of thousands of very short projections around 250 microns in length. Invisible to the naked eye and coated with vaccine, the projections can quickly deliver vaccine to immune cells.
Vaxxas also claims that the patches can deliver vaccine more efficiently — a positive when people around the world are clamouring for a vaccine against COVID-19. The company points to a recent clinical study in which their micropatch delivering a sixth of an influenza vaccine dose produced an immune response comparable to a full dose by intramuscular injection. A two-thirds dose by HD-MAP generated significantly faster and higher overall antibody responses.
Because a vaccine is dried onto the patch, the vaccines are stable outside of cold-chain (they do not have to be refridgerated), a potential answer to the question of how to keep a traditional COVID-19 vaccine cold in developing countries and even developed countries. Vaccines delivered through HD-MAP in the clinical study stayed stable at 40 oC (104 oF) for 12 months.



